Demystifying Hospital Pricing
I woke up the other day to a slew of text messages asking: "Did you see that executive order?" Most days, this might set off some alarms, but I had already seen the news. On June 24th, President Trump signed an executive order mandating hospitals and insurers to "publish prices that reflect what people pay for services." Notably, this latest directive aims to improve pricing transparency in healthcare.
Earlier this year though, the CMS, the largest government-sponsored payor in healthcare, required hospitals to publish charge prices, which meant little to the average consumers, especially considering that insurers rarely pay the full price to begin with.
As the go-to healthcare guy, I get a lot of questions ranging from which hospital to go to, to how to make medical bills go away - which I wish I knew the answer to! In particular, I get asked about pricing almost once a day, so let's dive deeper into that topic now...
For non-healthcare folks, here's how pricing works when you go to the hospital or the ER
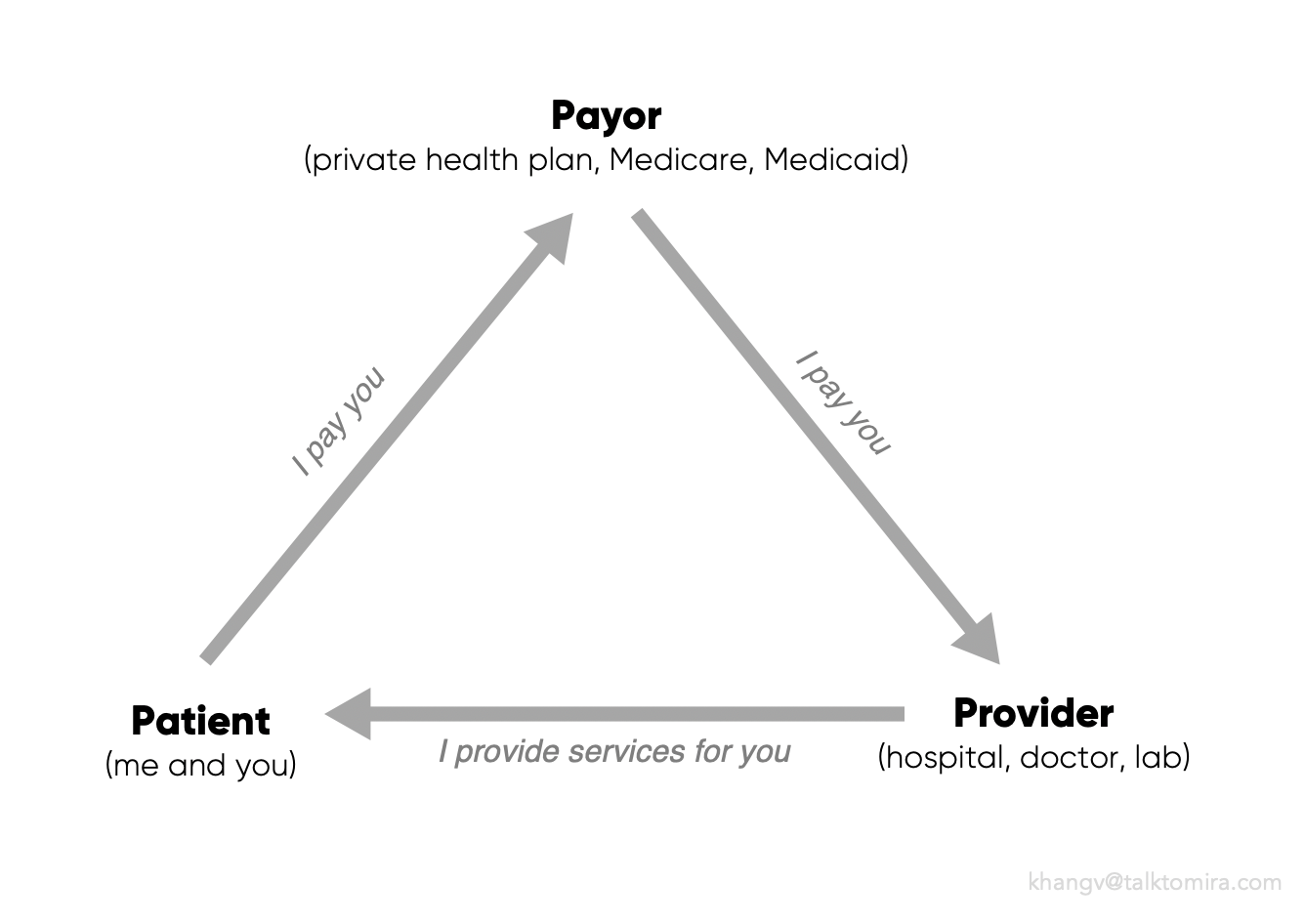
The first step is to understand the healthcare triangle.
Unlike going to the grocery store, in most cases, you're unable to "buy" healthcare yourself. Instead, you pay into a pool of cash, which is your insurance, with the hope that if something catastrophic happens, your insurance will cover it.
Working on your behalf, the insurer negotiates with hospitals to get you the best discounts off of the charge/full prices...supposedly.
While overly simplified, the triangle below depicts the three main stakeholders in a healthcare ecosystem (with suppliers and pharmaceutical companies excluded from the picture):

Get affordable doctor copay without paying insurance premiums
Join 39,000 people and get Mira, the best alternative to traditional insurance. Enroll and use immediately. Plans start at only $45/mo.
Khang T. Vuong received his Master of Healthcare Administration from the Milken Institute School of Public Health at the George Washington University. He was named Forbes Healthcare 2021 30 under 30. Vuong spoke at Stanford Medicine X, HIMSS conference, and served as a Fellow at the Bon Secours Health System.
